Palpation
of the Urinary Bladder
The full bladder in the adult projects up into the abdomen
and may be palpated through the anterior abdominal wall above the symphysis
pubis.
Bimanual palpation of the empty bladder with or
without a general anesthetic is an important method of examining the bladder. In
the male, one hand is placed on the anterior abdominal wall above the symphysis
pubis, and the gloved index finger of the other hand is inserted into the
rectum. From their knowledge of anatomy, students can see that the bladder wall
can be palpated between the examining fingers. In the female, an
abdominovaginal examination can be similarly made. In the child, the bladder is
in a higher position than in the adult because of the relatively smaller size
of the pelvis.
Bladder
Distention
The normal adult bladder has a capacity of about 500 mL. In the
presence of urinary obstruction in males, the bladder may become greatly
distended without permanent damage to the bladder wall; in such cases, it is
routinely possible to drain 1000 to 1200 mL of urine through a catheter.
Urinary
Retention
In adult males, urinary retention is commonly caused by
obstruction to the urethra by a benign or malignant enlargement of the prostate.
An acute urethritis or prostatitis can also be responsible. Acute retention
occurs much less frequently in females. The only anatomic cause of urinary
retention in females is acute inflammation around the urethra (e.g., from
herpes).
Suprapubic
Aspiration
As the bladder fills, the superior wall rises out of the
pelvis and peels the peritoneum off the posterior surface of the anterior abdominal
wall. In cases of acute retention of urine, when catheterization has failed, it
is possible to pass a needle into the bladder through the anterior abdominal
wall above the symphysis pubis, without entering the peritoneal cavity. This is
a simple method of draining off the urine in an emergency.
Cystoscopy
The mucous membrane of the bladder, the two ureteric
orifices, and the urethral meatus can easily be observed by means of a cystoscope.
With the bladder distended with fluid, an illuminated tube fitted with lenses
is introduced into the bladder through the urethra. Over the trigone, the
mucous membrane is pink and smooth. If the bladder is partially emptied, the
mucous membrane over the trigone remains smooth, but it is thrown into folds elsewhere.
The ureteric orifices are slitlike and eject a drop of urine at intervals of
about 1 minute. The interureteric ridge and the uvula vesicae can easily be
recognized.
Bladder
Injuries
The bladder may rupture intraperitoneally or
extraperitoneally. Intraperitoneal rupture usually involves the superior wall of
the bladder and occurs most commonly when the bladder is full and has extended
up into the abdomen. Urine and blood escape freely into the peritoneal cavity.
Extraperitoneal rupture involves the anterior part of the bladder wall below
the level of the peritoneal reflection; it most commonly occurs in fractures of
the pelvis when bony fragments pierce the bladder wall. Lower abdominal pain
and blood in the urine (hematuria) are found in most patients.
In young children, the bladder is an abdominal organ, so
abdominal trauma can injure the empty bladder.
Difficulty
with Micturition after Spinal Cord Injury
After injuries to the spinal cord, the nervous control of
micturition is disrupted.
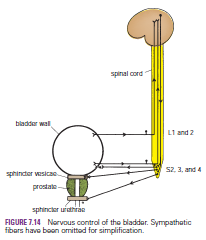
The normal bladder is innervated as follows:
■■
Sympathetic outflow is from the first and second lumbar segments of the spinal
cord. The sympathetic nerves inhibit contraction
of the detrusor muscle of the bladder wall and stimulate closure of the
sphincter vesicae.
■■
Parasympathetic outflow is from the second, third, and fourth sacral segments
of the spinal cord. The parasympathetic nerves stimulate the contraction of the
detrusor muscle of the bladder wall and inhibit the action of the sphincter
vesicae.
■■
Sensory nerve fibers enter the spinal cord at the above segments.