Vaginal
Examination
Digital examination of the vagina may provide the physician
with much valuable information concerning the health of the vaginal walls, the
uterus, and the surrounding structures
Injury
to the Perineum during Childbirth
The perineal body is a wedge of fibromuscular tissue that
lies between the lower part of the vagina and the anal canal. It is held in
position by the insertion of the perineal muscles and by the attachment of the
levator ani muscles. In the female, it is a much larger structure than in the
male, and it serves to support the posterior wall of the vagina. Damage by
laceration during childbirth can be followed by permanent weakness of the
pelvic floor.
Few women escape some injury to the birth canal during delivery. In most, this is little more than an abrasion of the posterior vaginal wall. Spontaneous delivery of the child with the patient unattended can result in a severe tear of the lower third of the posterior wall of the vagina, the perineal body, and overlying skin. In severe tears, the lacerations may extend backward into the anal canal and damage the external sphincter. In these cases, it is imperative that an accurate repair of the walls of the anal canal, vagina, and perineal body be undertaken as soon as possible.
Few women escape some injury to the birth canal during delivery. In most, this is little more than an abrasion of the posterior vaginal wall. Spontaneous delivery of the child with the patient unattended can result in a severe tear of the lower third of the posterior wall of the vagina, the perineal body, and overlying skin. In severe tears, the lacerations may extend backward into the anal canal and damage the external sphincter. In these cases, it is imperative that an accurate repair of the walls of the anal canal, vagina, and perineal body be undertaken as soon as possible.
In the management of childbirth, when it is obvious to the obstetrician
that the perineum will tear before the baby’s head emerges through the vaginal
orifice, a planned surgical incision is made through the perineal skin in a
posterolateral direction to avoid the anal sphincters. This procedure is known
as an episiotomy. Breech deliveries and forceps deliveries are usually preceded
by an episiotomy
.
.
Pudendal
Nerve Block
Area of Anesthesia
The area anesthetized is the skin of the perineum; this
nerve block does not, however, abolish sensation from the anterior part of the
perineum, which is innervated by the ilioinguinal nerve and the genitofemoral
nerve. Needless to say, it does not abolish pain from uterine contractions that
ascend to the spinal cord via the sympathetic afferent nerves.
Indications
During the second stage of a difficult labor, when the
presenting part of the fetus, usually the head, is descending through the
vulva, forceps delivery and episiotomy may be necessary
.
.
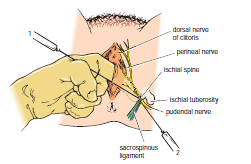
Transvaginal Procedure
The bony landmark used is the ischial spine . The index finger
is inserted through the vagina to palpate the ischial spine. The needle of the
syringe is then passed through the vaginal mucous membrane toward the ischial
spine. On passing through the sacrospinous ligament, the anesthetic solution is
injected around the pudendal nerve .
Perineal
Procedure
The bony landmark is the ischial tuberosity . The tuberosity
is palpated subcutaneously through the buttock, and the needle is introduced
into the pudendal canal along the medial side of the tuberosity. The canal lies
about 1 in. (2.5 cm) deep to the free surface of the ischial tuberosity. The
local anesthetic is then infiltrated around the pudendal nerve.