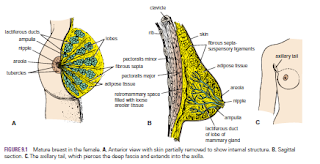
Breast
Examination
Because The breast is
one of the common sites of cancer in women. It is also the site of different
types of benign tumors and may be subject to acute inflammation and abscess
formation. For these reasons, the clinical personnel must be familiar with the
development, structure, and lymph drainage of this organ.
With the patient undressed to the waist and sitting upright,
the breasts are first inspected for symmetry. Some degree of asymmetry is
common and is the result of unequal breast development. Any swelling should be
noted. A swelling can be caused by an underlying tumor, a cyst, or abscess
formation. The nipples should be carefully examined for evidence of retraction.
A carcinoma within the breast substance can cause retraction of the nipple by
pulling on the lactiferous ducts. The patient is then asked to lie down so that
the breasts can be palpated against the underlying thoracic wall. Finally, the
patient is asked to sit up again and raise both arms above her head. With this
maneuver, a carcinoma tethered to the skin, the suspensory ligaments, or the
lactiferous ducts produces dimpling of the skin or retraction of the nipple.
Mammography
Mammography is a radiographic examination of the breast.
This technique is extensively used for screening the breasts for benign and
malignant tumors and cysts. Extremely low doses of x-rays are used so that the
dangers are minimal, and the examination can be repeated often. Its success is
based on the fact that a lesion measuring only a few millimeters in diameter can
be detected long before it is felt by clinical examination.
Breast
Abscess
during lactation An acute infection of the mammary gland may
occur. Pathogenic bacteria gain entrance to the breast tissue through a crack
in the nipple. Because of the presence of the fibrous septa, the infection
remains localized to one compartment or lobe to begin with. Abscesses should be
drained through a radial incision to avoid spreading of the infection into neighboring
compartments; a radial incision also minimizes the damage to the radially
arranged ducts.
Lymph
Drainage and Carcinoma of the Breast
The importance of knowing the lymph drainage of the breast
in relation to the spread of cancer from that organ cannot be overemphasized. The
lymph vessels from the medial quadrants of the breast pierce the 2nd, 3rd, and
4th intercostal spaces and enter the thorax to drain into the lymph nodes
alongside the internal thoracic artery. The lymph vessels from the lateral
quadrants of the breast drain into the anterior or pectoral group of axillary nodes.
It follows, therefore, that a cancer occurring in the lateral quadrants of the
breast tends to spread to the axillary nodes.
Thoracic metastases are difficult or impossible to treat,
but the lymph nodes of the axilla can be removed surgically. Approximately 60%
of carcinomas of the breast occur in the upper lateral quadrant. The lymphatic
spread of cancer to the opposite breast, to the abdominal cavity, or into lymph
nodes in the root of the neck is caused by obstruction of the normal lymphatic
pathways by malignant cells or destruction of lymph vessels by surgery or
radiotherapy. The cancer cells are swept along the lymph vessels and follow the
lymph stream. The entrance of cancer cells into the blood vessels accounts for
the metastases in distant bones.
In patients with localized cancer of the breast, most
surgeons do a simple mastectomy or a lumpectomy, followed by radiotherapy to
the axillary lymph nodes and/or hormone therapy. In patients with localized cancer
of the breast with early metastases in the axillary lymph nodes, most
authorities agree that radical mastectomy offers the best chance of cure. In
patients in whom the disease has already spread beyond these areas (e.g., into
the thorax), simple mastectomy, followed by radiotherapy or hormone therapy, is
the treatment of choice. Radical mastectomy is designed to remove the primary
tumor and the lymph vessels and nodes that drain the area. This means that the
breast and the associated structures containing the lymph vessels and nodes
must be removed en bloc. The excised mass is therefore made up of the
following: a large area of skin overlying the tumor and including the nipple;
all the breast tissue; the pectoralis major and associated fascia through which
the lymph vessels pass to the internal thoracic nodes; the pectoralis minor and
associated fascia related to the lymph vessels passing to the axilla; all the
fat, fascia, and lymph nodes in the axilla; and the fascia covering the upper
part of the rectus sheath, the serratus anterior, the subscapularis, and the
latissimus dorsi muscles. The axillary blood vessels, the brachial plexus, and
the nerves to the serratus anterior and the latissimus dorsi are preserved.
Some degree of postoperative edema of the arm is likely to follow such a
radical removal of the lymph vessels draining the upper limb. A modified form
of radical mastectomy for patients with clinically localized cancer is also a
common procedure and consists of a simple mastectomy in which the pectoral
muscles are left intact. The axillary lymph nodes, fat, and fascia are removed.
This procedure removes the primary tumor and permits pathologic examination of
the lymph nodes for possible metastases
Carcinoma
in the Male Breast
Carcinoma in the male breast accounts for about 1% of all
carcinomas of the breast. This fact tends to be overlooked when examining the
male patient.
Since the amount of breast tissue in the male is small, the tumor
can usually be felt with the flat of the examining hand in the early stages.
However, the prognosis is relatively poor in the male, because the carcinoma
cells can rapidly metastasize into the thorax through the small amount of
intervening tissue.