Brachial
Plexus
The nerves entering the upper limb provide the following
important functions: sensory innervation to the skin and deep structures, such
as the joints; motor innervation to the muscles; influence over the diameters
of the blood vessels by the sympathetic vasomotor nerves; and sympathetic
secretomotor supply to the sweat glands. At the root of the neck, the nerves
form a complicated plexus called the brachial plexus. This allows the
nerve fibers derived from different segments of the spinal cord to be arranged
and distributed efficiently in different nerve trunks to the various parts of
the upper limb. The brachial plexus is formed in the posterior triangle of the
neck by the union of the anterior rami of the 5th, 6th, 7th, and 8th cervical and
the 1st thoracic spinal nerves.
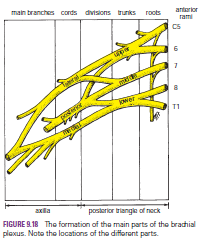
The plexus can be divided into roots, trunks, divisions,
and cords. The roots of C5 and 6 unite to form the upper trunk, the
root of C7 continues as the middle trunk, and the roots of C8 and T1
unite to form the lower trunk. Each trunk then divides into anterior and
posterior divisions. The anterior divisions of the upper and middle trunks
unite to form the lateral cord, the anterior division of the lower trunk
continues as the medial cord, and the posterior divisions of all three
trunks join to form the posterior cord.
The roots, trunks, and divisions of the brachial plexus
reside in the lower part of the posterior triangle of the neck and are fully
described on page XXX. The cords become arranged around the axillary artery in
the axilla. Here, the brachial plexus and the axillary artery and vein are
enclosed in the axillary sheath.
Cords of the Brachial Plexus All three cords of the
brachial plexus lie above and lateral to the first part of the axillary artery.
The medial cord crosses behind the artery to reach the medial side of the second
part of the artery . The posterior cord lies behind the second part of the
artery, and the lateral cord lies on the lateral side of the second part of the
artery . Thus, the cords of the plexus have the relationship to the second part
of the axillary artery that is indicated by their names.
Most branches of the cords that form the main nerve trunks
of the upper limb continue this relationship to the artery in its third part .
The branches of the different parts of the brachial
plexus are as follows:
■■ Roots
Dorsal scapular nerve (C5)
Long thoracic nerve (C5, 6, and 7)
■■ Upper
trunk
Nerve to subclavius (C5 and 6)
Suprascapular nerve (supplies the supraspinatus and
infraspinatus muscles)
■■ Lateral
cord
Lateral pectoral nerve
Musculocutaneous nerve
Lateral root of median nerve
■■ Medial
cord
Medial pectoral nerve
Medial cutaneous nerve of arm and medial cutaneous
nerve of forearm
Ulnar nerve
Medial root of median nerve
■■ Posterior
cord
Upper and lower subscapular nerves
Thoracodorsal nerve
Axillary nerve
The
Axillary Sheath and a Brachial Plexus Nerve Block
Because the axillary sheath encloses the axillary vessels
and the brachial plexus, a brachial plexus nerve block can easily be obtained.
The distal part of the sheath is closed with finger pressure, and a syringe
needle is inserted into the proximal part of the sheath. The anesthetic
solution is then injected into the sheath, and the solution is massaged along the
sheath to produce the nerve block. The position of the sheath can be verified by
feeling the pulsations of the third part of the axillary artery.